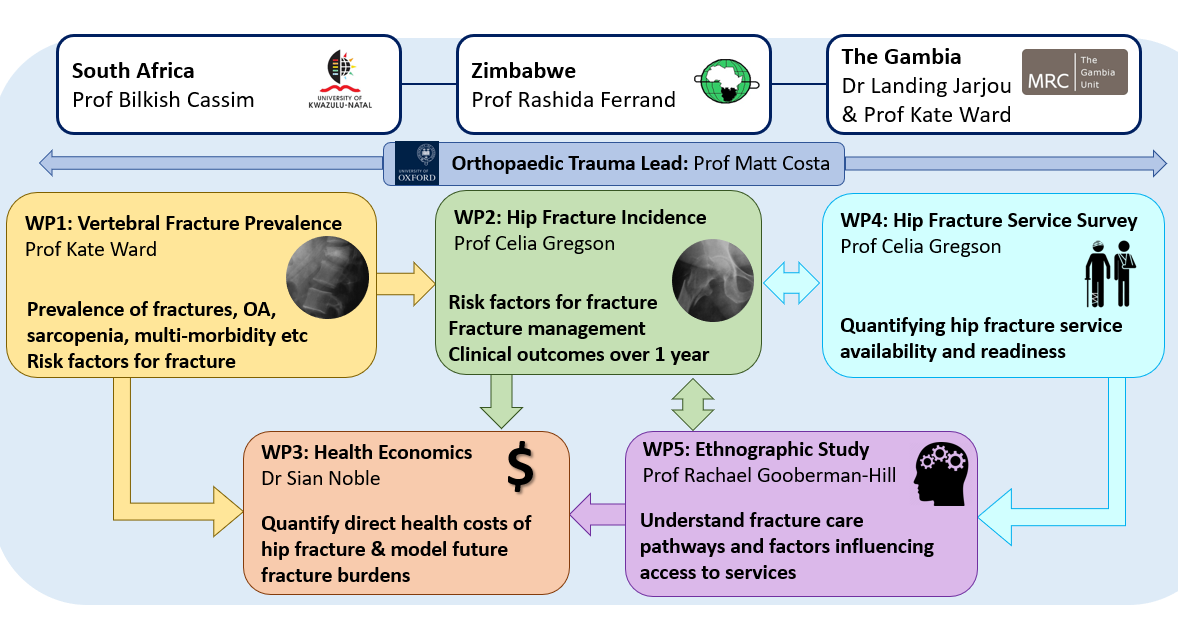
Figure 1: Overview of Study Design & Co-investigators
Aims and Approach
This study is an international mixed-methods study using cross-sectional and longitudinal study designs together with ethnographic study to investigate the epidemiology, economic impact, and ethnography of fractures in The Gambia, Zimbabwe, and SA. Within four workpackages (WP) we aim to address the following objectives:
WP1. Determine the epidemiology of vertebral fractures
a) Quantify vertebral fracture prevalence amongst men and women aged 40 years and older by community-based population surveys across urban, peri-urban, and rural settings.
b) Determine clinical risk factors for vertebral fractures, particularly the role of HIV and HIV-related factors, the role of traditional osteoporosis risk factors, and other co-morbidities, between individuals with and without fracture. We will further determine the prevalence of wider musculoskeletal morbidities, including osteoarthritis, sarcopenia and injurious falls, and associations with functional impairment in terms of activities of daily living (ADLs), and health-related quality-of-life (HR-QOL). Individuals surveyed in WP1(a) without a history of hip fracture, will provide an age and sex frequency-matched comparator group for the incident hip fracture population, identified in 2(b) below.
WP2. Determine the epidemiology of hip fractures
a) Determine hip fracture incidence in men and women aged 40 years and older. Understand risk factors, fracture mechanisms (determining the burden due to fragility relative to trauma), and management received (Zimbabwe and The Gambia only, as data recently published from South Africa 2)
b) Establish hip fracture outcomes over 12 months, including hospital length-of-stay, readmission, mortality, function in terms of ADLs, disability, and HR-QOL, and predictors of adverse outcomes.
WP3. Determine the health costs attributable to incident hip fractures and model future fracture burdens
a) Using high-quality patient and site-level cost data on healthcare in the year following hip fracture we will perform health economic analyses to determine the direct and indirect health costs and budget impact attributable to hip fracture care, informing decision makers on affordability of different care models.
b) We will establish the main predictors of healthcare costs using risk factors and outcomes recorded in WP2.
c) We will determine the cost-effectiveness of different pathways of care and cost-effectiveness-based intervention thresholds for the treatment of osteoporosis within these settings.
d) Combining data from WP1, WP2 and population projection data, we will model future fracture burdens and health costs predicted to be attributable to hip fracture within the region.
WP4. Quantify current hip fracture services for each country (WP4)
We will quantify current hip fracture services for each country, including types of facilities, fracture services, referral patterns, drug supplies/costs, staffing, equipment, and radiology using the modified WHO Service Availability & Readiness Assessment (SARA) survey framework.
WP5. Understand and characterise care pathways for hip fracture and identify factors that help and hinder set-up and implementation of fracture services (WP5)
If ultimately this research is to impact health policy and the configuration of fracture services in SSA, it is crucial to understand current health services and management practices to inform healthcare improvement strategies. We will characterise hip fracture services by ethnographic study in both urban and rural environments, aiming to understand:
a) Pathways to and through fracture care, including how people with fractures do or do not make it into and through current services.
b) Factors that help or hinder the implementation of fracture treatment services. We will explore and characterise decision rationales and barriers and facilitators to care delivery.
Expected impact
Greater understanding of fracture care will be able to inform health service policy and planning in SSA, for example it is intended that our findings will influence essential medicines availability, calibrate risk assessment tools for generalised clinical use, inform national clinical guidelines and advise health service development for the future.
Presentations by Celia Gregson and Kate Ward providing background and introduction to this project available here:
https://www.osteoporosis.foundation/educational-hub/material/webinars
References:
